Mississippi Today
Judge rejects evidence of suicide in denying new trial for woman convicted of murder
A trial judge has rejected the request of a mother of four for a new trial, despite the state's pathologist reversing his original ruling and saying the death was more likely a suicide.
“Nothing in Mississippi statutory and case law requires that the Forensic Pathologist must determine the manner of death to be homicide before a jury may convict a defendant of murder,” wrote Circuit Judge James Kitchens Jr.
A Clay County jury convicted Tameshia Shelton of murder in the 2009 shooting death of her sister's boyfriend, Danelle Young. Shelton, who was sentenced to life, won't be eligible for parole until 2043.
“Every day that passes represents an incalculable hardship to Ms. Shelton, to her children and her loved ones, as she serves her life in prison for a crime that never happened,” said her lawyer, Sandra Levick. “We will definitely appeal. We trust the higher court will correct this injustice.”
The prosecution never presented a motive for why Shelton, now 45, would have killed Young.
In April 2022, Kitchens presided over the last of three days of hearings over whether Shelton deserved a new trial. Those post-conviction hearings revealed evidence never shown to the jury, including an apparent suicide note Young wrote.
In 2009, forensic pathologist Dr. Liam Funte ruled Young's death a homicide, basing that decision on the trajectory of the bullet from the front of the chest to the back “without significant deviation to left or right.”
Under questioning by Levick at one hearing, Funte said at the time he had not seen that in a suicide, but he said he has seen such cases since and was “leaning toward suicide.”
In reversing the original ruling, he cited scientific studies on bullet trajectories in suicides and homicides. In one study, more than 36% of suicides had bullet trajectories that did not deviate to the left or right.
After a verbal argument in which Shelton's sister said she told Young that she didn't want to live with him, Young walked to Shelton's trailer.
Shelton told authorities that she was already in bed with her infant daughter when Young knocked on the window of the trailer. She went to the front door, and she said he told her that he only needed one bullet to kill a racoon.
She said she replied that he might need more than one bullet and loaded her .22 pistol and gave it to him.
When he failed to return, she said she went outside, found him collapsed on the gravel driveway and called 911.
In the autopsy report, Funte concluded the gun was fired from less than an inch away.
Both he and another forensic pathologist, Dr. Randall Frost, demonstrated at hearings how the small gun could fire a self-inflicted shot, following the same path the bullet traveled through Young's body.

Funte said he would now rule the death “undetermined.”
Kitchens never addressed either the demonstrations or the apparent suicide note in his 15-page decision. In that note, Young wrote, “I have no life without her [Shelton's sister]. … Tell [your daughter] Treasure about me one day. Bye. Bye.”
Under cross-examination at the post-conviction hearing by Special Assistant Attorney General Jackie Bost II, Funte acknowledged one scientific study showed that more than 82% of suicides by gunfire were shots to the head, while 16% were shots to the chest.
Other pathologists, who testified for the defense at the hearing, said Young's death should have been ruled a suicide or undetermined.
At trial, Funte cited the lack of history that Young had suicidal thoughts or attempts, but said he had since seen impulsive suicides with no such history.
Asked how many suicides he had seen that were impulsive, Funte replied between 15% and 20%, with studies that put that number beyond 20%.
Bost asked, “So, four out of five suicides are not impulsive?”
“Correct,” Funte replied.

During the hearing, Judge Kitchens said Funte's changed testimony “is probably the most damning to the conviction … That's hard to get around.”
But in his new ruling, the judge found no problem.
Although the last hearing took place in April 2022, Kitchens had yet to rule in the case when Shelton's lawyers complained to the Mississippi Supreme Court in November 2023. A clerk told justices that Kitchens should rule in December 2023.
When that didn't happen by Jan. 22, justices ordered Kitchens to complete an order in 45 days. He took 53 days.
Matt Steffey, professor of law at the Mississippi College School of Law, said both dynamics and legal reasons make it difficult to persuade a trial judge to reverse a conviction in a case that he presided over a trial.
During a trial, a defendant is presumed innocent, but after a conviction, the law presumes the defendant is guilty, Steffey said. “It's not enough to persuade a court that an error has been made.”
The defendant also has to prove the error likely impacted the verdict, he said. “This is a difficult standard to meet.”
Cognitive science shows how difficult it is to persuade people of their errors, and there are political dynamics as well, he said. “Trial judges are elected officials. Vacating convictions or ordering new trials can provide fodder for potential political opponents eager to claim a judge is insufficiently tough on crime and criminals.”
The simple truth is post-conviction relief offers “narrow grounds and a slim chance for success,” he said.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.
Mississippi Today
On this day in 1954
MAY 17, 1954

In Brown v. Board of Education and Bolling v. Sharpe, the U.S. Supreme Court unanimously ruled that the “separate but equal” doctrine in Plessy v. Ferguson was unconstitutional under the 14th Amendment, which guaranteed equal treatment under the law.
The historic decision brought an end to federal tolerance of racial segregation, ruling in the case of student Linda Brown, who was denied admission to her local elementary school in Topeka, Kansas, because of the color of her skin.
In Mississippi, segregationist leaders called the day “Black Monday” and took up the charge of the just-created white Citizens' Council to preserve racial segregation at all costs.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.
Mississippi Today
Every university but Delta State to increase tuition this year
Every university in Mississippi is increasing tuition in the fall except for Delta State University.
The new rates were approved by the governing board of the eight universities, the Institutions of Higher Learning Board of Trustees, at its regular meeting Thursday.
The average cost of tuition in Mississippi is now $8,833 a year, a roughly 3% increase from last year. Students can expect to pay tuition ranging from $7,942 a year at Mississippi Valley State University to $10,052 a year at Mississippi State University.
In recent years, universities have cited inflation and rising insurance costs as reasons for the tuition increases. At Thursday's meeting, the board heard a presentation on how property insurance is becoming more expensive for the eight universities as Mississippi sees more tornadoes and storms with severe wind and hail.
READ MORE: Tuition increases yet again at most public universities
But it's an ongoing trend. Mississippi's public universities have steadily increased tuition since 2000, putting the cost of college increasingly out of reach for the average Mississippi family. More than half of Mississippi college students graduated with an average of $29,714 in student debt in 2020, according to the Institution for College Access and Success.
At Delta State University, the president, Daniel Ennis, announced that he will attempt to avoid tuition increases as the regional college in the Mississippi Delta undergoes drastic budget cuts in an effort to become more financially sustainable.
“We will resist tuition increases so that our most economically vulnerable students can continue to have access to the opportunities that a college degree can provide,” he wrote in a memo to faculty and staff on Monday. “We will move beyond basic survival and into a place where we have the capacity to take better advantage of our undeniable strengths.”
Delta State didn't increase tuition last year, either. Officials have been concerned the university is becoming too pricey for the students it serves.
Tuition for the 2024-25 academic year, by school:
- Alcorn State University: $8,105
- Delta State University: $8,435
- Jackson State University: $8,690
- Mississippi State University: $10,052
- Mississippi University for Women: $8,392
- Mississippi Valley State University: $7,492
- University of Mississippi: $9,612
- University of Southern Mississippi: $9,888
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.
Mississippi Today
Federal panel prescribes new mental health strategy to curb maternal deaths

For help, call or text the National Maternal Mental Health Hotline at 1-833-TLC-MAMA (1-833-852-6262) or contact the 988 Suicide & Crisis Lifeline by dialing or texting “988.” Spanish-language services are also available.
BRIDGEPORT, Conn. — Milagros Aquino was trying to find a new place to live and had been struggling to get used to new foods after she moved to Bridgeport from Peru with her husband and young son in 2023.
When Aquino, now 31, got pregnant in May 2023, “instantly everything got so much worse than before,” she said. “I was so sad and lying in bed all day. I was really lost and just surviving.”
Aquino has lots of company.
Perinatal depression affects as many as 20% of women in the United States during pregnancy, the postpartum period, or both, according to studies. In some states, anxiety or depression afflicts nearly a quarter of new mothers or pregnant women.
Many women in the U.S. go untreated because there is no widely deployed system to screen for mental illness in mothers, despite widespread recommendations to do so. Experts say the lack of screening has driven higher rates of mental illness, suicide, and drug overdoses that are now the leading causes of death in the first year after a woman gives birth.
“This is a systemic issue, a medical issue, and a human rights issue,” said Lindsay R. Standeven, a perinatal psychiatrist and the clinical and education director of the Johns Hopkins Reproductive Mental Health Center.
Standeven said the root causes of the problem include racial and socioeconomic disparities in maternal care and a lack of support systems for new mothers. She also pointed a finger at a shortage of mental health professionals, insufficient maternal mental health training for providers, and insufficient reimbursement for mental health services. Finally, Standeven said, the problem is exacerbated by the absence of national maternity leave policies, and the access to weapons.
Those factors helped drive a 105% increase in postpartum depression from 2010 to 2021, according to the American Journal of Obstetrics & Gynecology.
For Aquino, it wasn't until the last weeks of her pregnancy, when she signed up for acupuncture to relieve her stress, that a social worker helped her get care through the Emme Coalition, which connects girls and women with financial help, mental health counseling services, and other resources.
Mothers diagnosed with perinatal depression or anxiety during or after pregnancy are at about three times the risk of suicidal behavior and six times the risk of suicide compared with mothers without a mood disorder, according to recent U.S. and international studies in JAMA Network Open and The BMJ.
The toll of the maternal mental health crisis is particularly acute in rural communities that have become maternity care deserts, as small hospitals close their labor and delivery units because of plummeting birth rates, or because of financial or staffing issues.
This week, the Maternal Mental Health Task Force — co-led by the Office on Women's Health and the Substance Abuse and Mental Health Services Administration and formed in September to respond to the problem — recommended creating maternity care centers that could serve as hubs of integrated care and birthing facilities by building upon the services and personnel already in communities.
The task force will soon determine what portions of the plan will require congressional action and funding to implement and what will be “low-hanging fruit,” said Joy Burkhard, a member of the task force and the executive director of the nonprofit Policy Center for Maternal Mental Health.
Burkhard said equitable access to care is essential. The task force recommended that federal officials identify areas where maternity centers should be placed based on data identifying the underserved. “Rural America,” she said, “is first and foremost.”
There are shortages of care in “unlikely areas,” including Los Angeles County, where some maternity wards have recently closed, said Burkhard. Urban areas that are underserved would also be eligible to get the new centers.
“All that mothers are asking for is maternity care that makes sense. Right now, none of that exists,” she said.
Several pilot programs are designed to help struggling mothers by training and equipping midwives and doulas, people who provide guidance and support to the mothers of newborns.
In Montana, rates of maternal depression before, during, and after pregnancy are higher than the national average. From 2017 to 2020, approximately 15% of mothers experienced postpartum depression and 27% experienced perinatal depression, according to the Montana Pregnancy Risk Assessment Monitoring System. The state had the sixth-highest maternal mortality rate in the country in 2019, when it received a federal grant to begin training doulas.
To date, the program has trained 108 doulas, many of whom are Native American. Native Americans make up 6.6% of Montana's population. Indigenous people, particularly those in rural areas, have twice the national rate of severe maternal morbidity and mortality compared with white women, according to a study in Obstetrics and Gynecology.
Stephanie Fitch, grant manager at Montana Obstetrics & Maternal Support at Billings Clinic, said training doulas “has the potential to counter systemic barriers that disproportionately impact our tribal communities and improve overall community health.”
Twelve states and Washington, D.C., have Medicaid coverage for doula care, according to the National Health Law Program. They are California, Florida, Maryland, Massachusetts, Michigan, Minnesota, Nevada, New Jersey, Oklahoma, Oregon, Rhode Island, and Virginia. Medicaid pays for about 41% of births in the U.S., according to the Centers for Disease Control and Prevention.
Jacqueline Carrizo, a doula assigned to Aquino through the Emme Coalition, played an important role in Aquino's recovery. Aquino said she couldn't have imagined going through such a “dark time alone.” With Carrizo's support, “I could make it,” she said.
Genetic and environmental factors, or a past mental health disorder, can increase the risk of depression or anxiety during pregnancy. But mood disorders can happen to anyone.
Teresa Martinez, 30, of Price, Utah, had struggled with anxiety and infertility for years before she conceived her first child. The joy and relief of giving birth to her son in 2012 were short-lived.
Without warning, “a dark cloud came over me,” she said.
Martinez was afraid to tell her husband. “As a woman, you feel so much pressure and you don't want that stigma of not being a good mom,” she said.
In recent years, programs around the country have started to help doctors recognize mothers' mood disorders and learn how to help them before any harm is done.
One of the most successful is the Massachusetts Child Psychiatry Access Program for Moms, which began a decade ago and has since spread to 29 states. The program, supported by federal and state funding, provides tools and training for physicians and other providers to screen and identify disorders, triage patients, and offer treatment options.
But the expansion of maternal mental health programs is taking place amid sparse resources in much of rural America. Many programs across the country have run out of money.
The federal task force proposed that Congress fund and create consultation programs similar to the one in Massachusetts, but not to replace the ones already in place, said Burkhard.
In April, Missouri became the latest state to adopt the Massachusetts model. Women on Medicaid in Missouri are 10 times as likely to die within one year of pregnancy as those with private insurance. From 2018 through 2020, an average of 70 Missouri women died each year while pregnant or within one year of giving birth, according to state government statistics.
Wendy Ell, executive director of the Maternal Health Access Project in Missouri, called her service a “lifesaving resource” that is free and easy to access for any health care provider in the state who sees patients in the perinatal period.
About 50 health care providers have signed up for Ell's program since it began. Within 30 minutes of a request, the providers can consult over the phone with one of three perinatal psychiatrists. But while the doctors can get help from the psychiatrists, mental health resources for patients are not as readily available.
The task force called for federal funding to train more mental health providers and place them in high-need areas like Missouri. The task force also recommended training and certifying a more diverse workforce of community mental health workers, patient navigators, doulas, and peer support specialists in areas where they are most needed.
A new voluntary curriculum in reproductive psychiatry is designed to help psychiatry residents, fellows, and mental health practitioners who may have little or no training or education about the management of psychiatric illness in the perinatal period. A small study found that the curriculum significantly improved psychiatrists' ability to treat perinatal women with mental illness, said Standeven, who contributed to the training program and is one of the study's authors.
Nancy Byatt, a perinatal psychiatrist at the University of Massachusetts Chan School of Medicine who led the launch of the Massachusetts Child Psychiatry Access Program for Moms in 2014, said there is still a lot of work to do.
“I think that the most important thing is that we have made a lot of progress and, in that sense, I am kind of hopeful,” Byatt said.
Cheryl Platzman Weinstock's reporting is supported by a grant from the National Institute for Health Care Management Foundation. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.
Did you miss our previous article…
https://www.biloxinewsevents.com/?p=359245
-
SuperTalk FM4 days ago
Martin Lawrence making 3 stops in Mississippi on comedy tour
-
Our Mississippi Home3 days ago
Beat the Heat with Mississippi’s Best Waterparks
-
Mississippi Today7 days ago
Lawmakers may have to return to Capitol May 14 to override Gov. Tate Reeves’ potential vetoes
-
Our Mississippi Home4 days ago
Charlie’s U-Pik: Opening Soon for the Summer Season
-
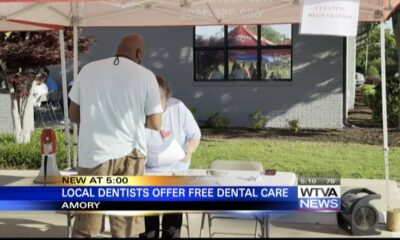
Mississippi News Video6 days ago
Local dentists offer free dental care in Amory
-
Kaiser Health News3 days ago
Medicaid ‘Unwinding’ Decried as Biased Against Disabled People
-
Mississippi News Video2 days ago
Jackson has a gang problem
-
Mississippi News7 days ago
Bond set for West Point couple accused of killing their child




























![HIGH SCHOOL SOFTBALL: Vancleave @ East Central (5/9/2024) [5A Playoffs, South State]](https://www.biloxinewsevents.com/wp-content/uploads/2024/05/1715460379_maxresdefault-80x80.jpg)