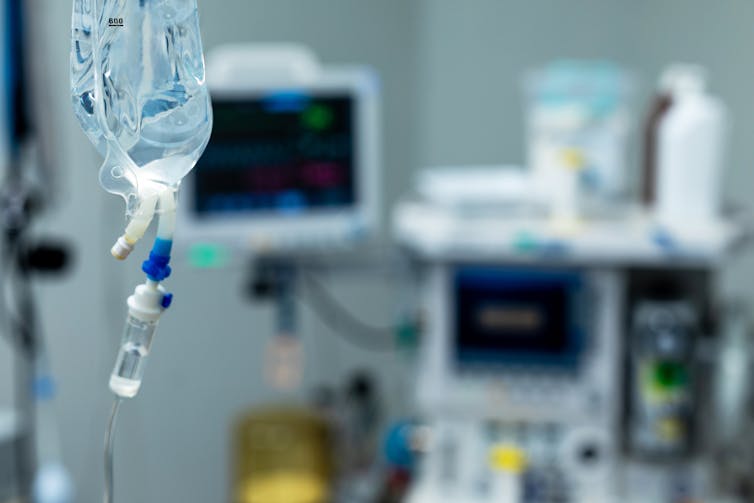
Opioids have been an essential part of anesthesia, but they aren’t the only way to manage pain.
Heather Margonari, University of Pittsburgh; Jacques E. Chelly, University of Pittsburgh, and Shiv K. Goel, University of Pittsburgh
The opioid crisis remains a significant public health challenge in the United States. In 2022, over 2.5 million American adults had an opioid use disorder, and opioids accounted for nearly 76% of overdose deaths.
Some patients are fearful of using opioids after surgery due to concerns about dependence and potential side effects, even when appropriately prescribed by a doctor to manage pain. Surgery is often the first time patients receive an opioid prescription, and their widespread use raises concerns about patients becoming long-term users. Leftover pills from a patient’s prescriptions may also be misused.
Researchers like us are working to develop a personalized and comprehensive surgical experience that doesn’t use opioids. Our approach to opioid-free surgery addresses both physical and emotional well-being through effective anesthesia and complementary pain-management techniques.
What is opioid-free anesthesia?
Clinicians have used morphine and other opioids to manage pain for thousands of years. These drugs remain integral to anesthesia.
Most surgical procedures use a strategy called balanced anesthesia, which combines drugs that induce sleep and relax muscles with opioids to control pain. However, using opioids in anesthesia can lead to unwanted side effects, such as serious cardiac and respiratory problems, nausea and vomiting, and digestive issues.
Concerns over these adverse effects and the opioid crisis have fueled the development of opioid-free anesthesia. This approach uses non-opioid drugs to relieve pain before, during and after surgery while minimizing the risk of side effects and dependency. Studies have shown that opioid-free anesthesia can provide similar levels of pain relief to traditional methods using opioids.
Opioid-free anesthesia is currently based on a multimodal approach. This means treatments are designed to target various pain receptors beyond opioid receptors in the spinal cord. Multimodal analgesia uses a combination of at least two medications or anesthetic techniques, each relieving pain through distinct mechanisms. The aim is to effectively block or modulate pain signals from the brain, spinal cord and the nerves of the body.
Balanced anesthesia combines a number of different drugs to ensure a smooth surgery.
For instance, nonsteroidal anti-inflammatory drugs, or NSAIDs, such as ibuprofen work by inhibiting COX enzymes that promote inflammation. Acetaminophen, or Tylenol, similarly inhibits COX enzymes. While both acetaminophen and NSAIDs primarily target pain at the surgical site, they can also exert effects at the spinal level after several days of use.
A class of drugs called gabapentinoids, which include gabapentin and pregabalin, target certain proteins to dampen nerve signal transmission. This decreases neuropathic pain by reducing nerve inflammation.
The anesthetic ketamine disrupts pain pathways that contribute to a condition called central sensitization. This disorder occurs when nerve cells in the spinal cord and brain amplify pain signals even when the original injury or source of pain has healed. As a result, normal sensations such as light touch or mild pressure may be perceived as painful, and painful stimuli may feel more intense than usual. By lessening pain sensitivity, ketamine can help reduce the risk of chronic pain.
Regional anesthesia involves injecting local anesthetics near nerves to block pain signals to the brain. This method allows patients to remain awake but pain-free in the numbed area, reducing the need for general anesthesia and its side effects. Common regional techniques include epidurals, spinal anesthesia and nerve blocks.
By activating different pain pathways simultaneously, multimodal approaches aim to enhance pain relief synergistically.
Psychology of pain perception
Psychological factors can significantly influence a patient’s perception of pain. Research indicates that mental health conditions such as anxiety, depression and sleep disturbances can increase pain levels by up to 50%. This suggests that addressing mood and sleep issues can be essential for pain management and improving overall patient well-being.
Psychological states can intensify the perception of pain by significantly influencing the neural pathways related to pain processing. For example, anxiety and stress activate the body’s fight or flight response, prompting the release of stress hormones that heighten nerve sensitivity. This can make pain feel more intense. Research has also found that higher anxiety levels before surgery are linked to increased anesthesia use during surgery and opioid consumption after surgery.
Addressing pain before an operation can make patients feel better post-op.
Complementary and alternative techniques that address psychological factors can reduce pain and opioid use by modulating pain transmission in the nervous system and activating neurochemical pathways that promote pain relief.
For example, aromatherapy uses essential oils to stimulate the olfactory system. This can help reduce pain perception and enhance overall well-being by evoking emotional responses and promoting relaxation.
Music therapy stimulates the auditory system, which can distract patients from pain, lower anxiety levels and foster emotional healing. This can ultimately lead to reduced pain perception.
Relaxation exercises, such as deep breathing and progressive muscle relaxation, activate the parasympathetic nervous system and help promote a state of rest. Engaging the parasympathetic system helps the body conserve energy, slow your heart rate, lower blood pressure and relieve muscle tension. This can lead to decreased pain sensitivity by promoting a state of calmness.
Acupuncture involves inserting thin needles into specific body points, stimulating the release of endorphins and other neurotransmitters. These molecules can interrupt pain signals and promote healing processes within the body.
Moving toward opioid-free surgery
Transitioning away from opioids in surgery requires a shift in both practice and mindset across the entire health care team. Beyond anesthesiologists, other providers, including surgeons, nurses and medical trainees, also use opioids in patient care. All providers would need to be open to using alternative pain management techniques throughout the surgical process.
In response to the increasing patient demand for opioid-free surgical care, our team at the University of Pittsburgh Medical Center launched the patient-initiated Opioid-Free Surgical Pain Management Program in May 2024. To address both the physical and emotional dimensions of pain while optimizing recovery and safety, we recruited surgeons, anesthesiologists, nurses, pharmacists and hospital administrators to participate in the initiative.
Over the course of six months, our team enrolled 109 patients, 79 of whom successfully underwent surgeries without opioids. Barriers to participating in the program included patient perception of severe pain, inadequately addressing stress and anxiety before the operation and limited education in the department about the program.
However, subsequent refinements to the program – such as giving patients muscle relaxants while they were recovering from anesthesia – improved participation and reduced opioid use. Importantly, none of the 19 patients who received opioids while recovering in the hospital post-op required further opioid prescriptions at discharge.
These results reflect the promise of our pathway to minimize reliance on opioids while ensuring effective pain management. Enhanced psychological support for patients and education for providers in surgery departments can broaden the effectiveness of a comprehensive approach to managing pain.
Heather Margonari, Lead Coordinator for the Opioid Free Pathway, University of Pittsburgh; Jacques E. Chelly, Professor of Anesthesiology, Perioperative Medicine and Orthopedic Surgery, University of Pittsburgh, and Shiv K. Goel, Clinical Associate Professor of Anesthesiology, University of Pittsburgh
This article is republished from The Conversation under a Creative Commons license. Read the original article.