Kaiser Health News
ER’s Error Lands a 4-Year-Old in Collections (For Care He Didn’t Receive)
by Daniel Chang
Wed, 29 Mar 2023 09:00:00 +0000
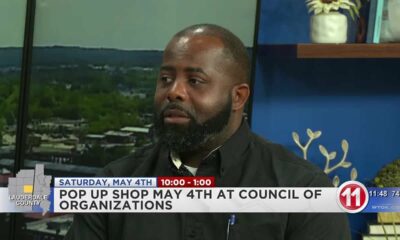
Dr. Sara McLin thought she made the right choice by going to an in-network emergency room near her Florida home after her 4-year-old burned his hand on a stove last Memorial Day weekend.
Her family is insured through her husband's employer, HCA Healthcare, a Nashville-based health system that operates more hospitals than any other system in the nation. So McLin knew that a nearby stand-alone emergency room, HCA Florida Lutz Emergency, would be in their plan's provider network.
But McLin said a doctor there told her she couldn't treat her son, Keeling, because he had second- and third-degree burns that needed a higher level of care. The doctor referred them to the burn center at HCA Florida Blake Hospital, about a 90-minute drive away.
McLin, who is a dentist, said the doctor told her the stand-alone ER would not charge for the visit because they did not provide treatment.
“I don't remember exactly how she phrased it. But something along the lines of, ‘Well, we won't even call this a visit, because we can't do anything,'” McLin said.
At Blake Hospital, she said, a doctor diagnosed Keeling with a second-degree burn, drained the blisters, bandaged his hand, and sent them home with instructions on how to care for the wound.
“I didn't think anything more of it,” McLin said.
Then the bills came.
The Patient: Keeling McLin, now 5, is covered by UnitedHealthcare through his father's employer.
Medical Service: At the stand-alone emergency room, a physician assessed Keeling and sent him to another facility for treatment. “Keeling needs a burn center,” the doctor wrote in the record of his visit.
Service Provider: Envision Physician Services, which employed the emergency room physician at HCA Florida Lutz Emergency in Lutz, Florida, near Tampa, and HCA Florida Trinity Hospital, the main, for-profit hospital to which the stand-alone emergency room belonged.
Total Bill: For the emergency room visit, Envision Physician Services billed $829 to insurance and about $72 to the family. HCA Florida Trinity Hospital billed Keeling about $129, noting it had applied an “uninsured discount.” An itemization showed the original charge had been nearly $1,509 before adjustments and discounts.
What Gives: The stand-alone emergency room and ER doctor, who saw Keeling but referred him to another hospital, billed for his visit. But McLin soon learned she was unable to dispute some of the charges — because her young child's name was on one of the bills, not hers.
Months after the ER visit, McLin received a bill addressed to the “parents of Keeling McLin” from Envision Physician Services, the provider staffing service that employed the ER doctor at Lutz. McLin recalled the doctor's promise that they would not be billed. “I should have made them write something down to that effect,” she said.
She said she called her insurer, UnitedHealthcare, and a representative told her not to pay the bill.
She received an insurance statement that identified the bill from Envision's doctor — an out-of-network provider working in an in-network emergency room — as a “surprise bill” for which the provider may charge only copays or other cost-sharing costs under federal law. McLin said she had not heard anything since then about the bill.
After being contacted by KHN, Aliese Polk, an Envision spokesperson, said in an email that Envision would waive the debt, apologizing to Keeling's family “for the misunderstanding.”
She described the ER doctor's evaluation, determination, and referral as a medical service. She said the bill was for cost sharing for the visit — not the difference between what the doctor charged and what insurance paid, as the law prohibits.
“We recognize the patient's family may have understood at the time of treatment that there would be no charge for the visit, including the medical service provided by our physician,” Polk said. “Unfortunately, this courtesy adjustment was not captured when the claim was processed.”
Maria Gordon Shydlo, a UnitedHealthcare spokesperson, said the insurer believed the matter had been resolved and did not follow up on requests for an interview, even after McLin waived federal health privacy protections, which would allow the insurer to speak to the reporter about the case.
McLin also received a bill from HCA Florida Trinity Hospital for its stand-alone ER at Lutz and decided to dispute the charges.
But after calling the hospital to appeal, McLin said, the billing department would not discuss the debt with her because the statement was in her young son's name.
“They had him as the guarantor,” McLin said. Unlike Envision, which billed Keeling's parents and their insurance, McLin said the hospital listed the child as “unemployed, uninsured.”
The child's ER record also included his date of birth and doctor's notes referencing his age. McLin said she wrote to HCA in November asking to appeal the bill and that a billing representative told her over the phone that it would put the debt on hold and review the dispute.
“I never heard anything back and assumed we were good,” McLin said.
Then, in January, she received a letter from Medicredit, a collection agency and an HCA subsidiary, stating that Keeling owed $129 and that he had until mid-February to contest the debt. KHN was unable to make contact with Medicredit representatives, and HCA Healthcare did not respond to requests for comment from its subsidiary.
Once again, Sara McLin's name was not on the debt collector's letter, and she said Medicredit representatives refused to discuss the debt with her because it was in her son's name. She said she called HCA, too. “They said, ‘We can't help you. We don't have the case anymore,'” she said.
Erin Fuse Brown, a law professor and director of the Center for Law, Health & Society at Georgia State University, said McLin did everything right and that it is unusual for a parent to be barred from discussing a debt related to their minor child.
“The fact that the hospital wouldn't even talk to her strikes me as the part that is absurd. It's absurd as a business matter. It's absurd as a privacy matter,” Fuse Brown said, adding that federal health privacy laws allow a parent or legal guardian to access their dependent's medical information.
Fuse Brown said the hospital should have been able to correct the error quickly with more information, such as a birth certificate or other document establishing that McLin was Keeling's parent. At the very least, she said, it could have given McLin notice before sending the bill to collections.
“You get the feeling that it's this large, automated process, that there's no human to get through to, that there's no human to talk to and override the mistake,” Fuse Brown said. “Maybe it's routine, but she couldn't even talk to someone to correct a correctable billing error, and then the system just steamrolls over the patient.”
The Resolution: When the collection agency's deadline passed without resolution, McLin said she felt frustrated. “Nobody can explain to me who has to approve talking to me,” she said. “I don't know who that person is or what the process is.”
After KHN contacted the health system, HCA Healthcare canceled the family's debt. HCA representatives declined to be interviewed on the record despite also receiving a privacy waiver from McLin.
“We have attempted to contact Mrs. McLin to apologize to her for the inconvenience this has caused her and to let her know that there is a zero balance on the account,” Debra McKell, marketing director for HCA West Florida Division, said in an email on March 3. “We also will be sharing with her that we are reviewing our processes to ensure this does not happen again.”
McLin later received a letter from HCA stating that the account had been cleared. She also said she received a call from a customer service representative informing her that the debt had not been reported to any credit agencies.
She said she was pleased, but that patients should not have to struggle to correct a billing error before it is sent to a collection agency and potentially ruins their credit.
“It's the principle of the thing that's annoying me at this point,” she said.
The Takeaway: Though the notion of a debt collector pursuing a 4-year-old boy may seem farcical, it happens. When seeking medical care for a minor, it is important for the parent or guardian to ensure their name is listed as the responsible party.
Consumers who find themselves fighting a medical billing error need to “think like a lawyer,” Fuse Brown said, including documenting every interaction with the debt collector, getting any promises in writing, and recording phone calls. (State laws vary about how many parties on a call must give permission to record a conversation.)
Patients do not have to give up once a bill goes to collections, Fuse Brown said. “Once you hear from a debt collector, it's not like the game is over and you lose,” she said. “Consumers do have rights.”
François de Brantes, a home health company executive and expert on how money flows through the health care system, said that hospital billing errors are not uncommon but that he had never heard of a situation like the one McLin experienced. He called it “puzzling” that HCA would issue a formal claim in a dependent child's name.
De Brantes said those in a similar situation should also ensure that the collection agency removes any record of a debt against a minor to protect the child's financial future.
“This stuff happens, where you have children who are improperly billed for stuff that they shouldn't be billed, and they end up in collection,” he said. “Then the kid finds themselves with a collection record and they can't get loans in the future, potentially student loans.”
Bill of the Month is a crowdsourced investigation by KHN and NPR that dissects and explains medical bills. Do you have an interesting medical bill you want to share with us? Tell us about it!
By: Daniel Chang
Title: ER's Error Lands a 4-Year-Old in Collections (For Care He Didn't Receive)
Sourced From: khn.org/news/article/hospital-sent-4-year-old-to-collections-emergency-room/
Published Date: Wed, 29 Mar 2023 09:00:00 +0000
Kaiser Health News
Mandatory Reporting Laws Meant To Protect Children Get Another Look
Kristin Jones
Thu, 25 Apr 2024 09:00:00 +0000
More than 60 years ago, policymakers in Colorado embraced the idea that early intervention could prevent child abuse and save lives. The state's requirement that certain professionals tell officials when they suspect a child has been abused or neglected was among the first mandatory reporting laws in the nation.
Since then, mandatory reporting laws have expanded nationally to include more types of maltreatment — including neglect, which now accounts for most reports — and have increased the number of professions required to report. In some states, all adults are required to report what they suspect may be abuse or neglect.
But now there are efforts in Colorado and other states to roll back these laws, saying the result has been too many unfounded reports, and that they disproportionately harm families that are poor, Black, or Indigenous, or have members with disabilities.
“There's a long, depressing history based on the approach that our primary response to a struggling family is reporting,” said Mical Raz, a physician and historian at the University of Rochester in New York. “There's now a wealth of evidence that demonstrates that more reporting is not associated with better outcomes for children.”
Stephanie Villafuerte, Colorado's child protection ombudsman, oversees a task force to reexamine the state's mandatory reporting laws. She said the group is seeking to balance a need to report legitimate cases of abuse and neglect with a desire to weed out inappropriate reports.
“This is designed to help individuals who are disproportionately impacted,” Villafuerte said. “I'm hoping it's the combination of these efforts that could make a difference.”
Some critics worry that changes to the law could result in missed cases of abuse. Medical and child care workers on the task force have expressed concern about legal liability. While it's rare for people to be criminally charged for failure to report, they can also face civil liability or professional repercussions, including threats to their licenses.
Being reported to child protective services is becoming increasingly common. More than 1 in 3 children in the United States will be the subject of a child abuse and neglect investigation by the time they turn 18, according to the most frequently cited estimate, a 2017 study funded by the Department of Health and Human Services' Children's Bureau.
Black and Native American families, poor families, and parents or children with disabilities experience even more oversight. Research has found that, among these groups, parents are more likely to lose parental rights and children are more likely to wind up in foster care.
In an overwhelming majority of investigations, no abuse or neglect is substantiated. Nonetheless, researchers who study how these investigations affect families describe them as terrifying and isolating.
In Colorado, the number of child abuse and neglect reports has increased 42% in the past decade and reached a record 117,762 last year, according to state data. Roughly 100,000 other calls to the hotline weren't counted as reports because they were requests for information or were about matters like child support or adult protection, said officials from the Colorado Department of Human Services.
The increase in reports can be traced to a policy of encouraging a broad array of professionals — including school and medical staff, therapists, coaches, clergy members, firefighters, veterinarians, dentists, and social workers — to call a hotline whenever they have a concern.
These calls don't reflect a surge in mistreatment. More than two-thirds of the reports received by agencies in Colorado don't meet the threshold for investigation. Of the children whose cases are assessed, 21% are found to have experienced abuse or neglect. The actual number of substantiated cases has not risen over the past decade.
While studies do not demonstrate that mandatory reporting laws keep children safe, the Colorado task force reported in January, there is evidence of harm. “Mandatory reporting disproportionately impacts families of color” — initiating contact between child protection services and families who routinely do not present concerns of abuse or neglect, the task force said.
The task force said it is analyzing whether better screening might mitigate “the disproportionate impact of mandatory reporting on under-resourced communities, communities of color and persons with disabilities.”
The task force pointed out that the only way to report concerns about a child is with a formal report to a hotline. Yet many of those calls are not to report abuse at all but rather attempts to connect children and families with resources like food or housing assistance.
Hotline callers may mean to help, but the families who are the subjects of mistaken reports of abuse and neglect rarely see it that way.
That includes Meighen Lovelace, a rural Colorado resident who asked KFF Health News not to disclose their hometown for fear of attracting unwanted attention from local officials. For Lovelace's daughter, who is neurodivergent and has physical disabilities, the reports started when she entered preschool at age 4 in 2015. The teachers and medical providers making the reports frequently suggested that the county human services agency could assist Lovelace's family. But the investigations that followed were invasive and traumatic.
“Our biggest looming fear is, ‘Are you going to take our children away?'” said Lovelace, who is an advocate for the Colorado Cross-Disability Coalition, an organization that lobbies for the civil rights of people with disabilities. “We're afraid to ask for help. It's keeping us from entering services because of the fear of child welfare.”
State and county human services officials said they could not comment on specific cases.
The Colorado task force plans to suggest clarifying the definitions of abuse and neglect under the state's mandatory reporting statute. Mandatory reporters should not “make a report solely due to a family/child's race, class or gender,” nor because of inadequate housing, furnishings, income or clothing. Also, there should not be a report based solely on the “disability status of the minor, parent or guardian,” according to the group's draft recommendation.
The task force plans to recommend additional training for mandatory reporters, help for professionals who are deciding whether to make a call, and an alternative phone number, or “warmline,” for cases in which callers believe a family needs material assistance, rather than surveillance.
Critics say such changes could leave more children vulnerable to unreported abuse.
“I'm concerned about adding systems such as the warmline, that kids who are in real danger are going to slip through the cracks and not be helped,” said Hollynd Hoskins, an attorney who represents victims of child abuse. Hoskins has sued professionals who fail to report their suspicions.
The Colorado task force includes health and education officials, prosecutors, victim advocates, county child welfare representatives and attorneys, as well as five people who have experience in the child welfare system. It intends to finalize its recommendations by early next year in the hope that state legislators will consider policy changes in 2025. Implementation of any new laws could take several years.
Colorado is one of several states — including New York and California — that have recently considered changes to restrain, rather than expand, reporting of abuse. In New York City, teachers are being trained to think twice before making a report, while New York state introduced a warmline to help connect families with resources like housing and child care. In California, a state task force aimed at shifting “mandated reporting to community supporting” is planning recommendations similar to Colorado's.
Among those advocating for change are people with experience in the child welfare system. They include Maleeka Jihad, who leads the Denver-based MJCF Coalition, which advocates for the abolition of mandatory reporting along with the rest of the child welfare system, citing its damage to Black, Native American, and Latino communities.
“Mandatory reporting is another form of keeping us policed and surveillanced by whiteness,” said Jihad, who as a child was taken from the care of a loving parent and placed temporarily into the foster system. Reform isn't enough, she said. “We know what we need, and it's usually funding and resources.”
Some of these resources — like affordable housing and child care — don't exist at a level sufficient for all the Colorado families that need them, Jihad said.
Other services are out there, but it's a matter of finding them. Lovelace said the reports ebbed after the family got the help it needed, in the form of a Medicaid waiver that paid for specialized care for their daughter's disabilities. Their daughter is now in seventh grade and doing well.
None of the caseworkers who visited the family ever mentioned the waiver, Lovelace said. “I really think they didn't know about it.”
——————————
By: Kristin Jones
Title: Mandatory Reporting Laws Meant To Protect Children Get Another Look
Sourced From: kffhealthnews.org/news/article/child-abuse-mandatory-reporting-laws-colorado/
Published Date: Thu, 25 Apr 2024 09:00:00 +0000
Did you miss our previous article…
https://www.biloxinewsevents.com/genetics-studies-have-a-diversity-problem-that-researchers-struggle-to-fix/
Kaiser Health News
Genetics Studies Have a Diversity Problem That Researchers Struggle To Fix
Lauren Sausser
Thu, 25 Apr 2024 09:00:00 +0000
CHARLESTON, S.C. — When he recently walked into the dental clinic at the Medical University of South Carolina donning a bright-blue pullover with “In Our DNA SC” embroidered prominently on the front, Lee Moultrie said, two Black women stopped him to ask questions.
“It's a walking billboard,” said Moultrie, a health care advocate who serves on the community advisory board for In Our DNA SC, a study underway at the university that aims to enroll 100,000 South Carolinians — including a representative percentage of Black people — in genetics research. The goal is to better understand how genes affect health risks such as cancer and heart disease.
Moultrie, who is Black and has participated in the research project himself, used the opportunity at the dental clinic to encourage the women to sign up and contribute their DNA. He keeps brochures about the study in his car and at the barbershop he visits weekly for this reason. It's one way he wants to help solve a problem that has plagued the field of genetics research for decades: The data is based mostly on DNA from white people.
Project leaders in Charleston told KFF Health News in 2022 that they hoped to enroll participants who reflect the demographic diversity of South Carolina, where just under 27% of residents identify as Black or African American. To date, though, they've failed to hit that mark. Only about 12% of the project's participants who provided sociodemographic data identify as Black, while an additional 5% have identified as belonging to another racial minority group.
“We'd like to be a lot more diverse,” acknowledged Daniel Judge, principal investigator for the study and a cardiovascular genetics specialist at the Medical University of South Carolina.
Lack of diversity in genetics research has real health care implications. Since the completion more than 20 years ago of the Human Genome Project, which mapped most human genes for the first time, close to 90% of genomics studies have been conducted using DNA from participants of European descent, research shows. And while human beings of all races and ancestries are more than 99% genetically identical, even small differences in genes can spell big differences in health outcomes.
“Precision medicine” is a term used to describe how genetics can improve the way diseases are diagnosed and treated by considering a person's DNA, environment, and lifestyle. But if this emerging field of health care is based on research involving mostly white people, “it could lead to mistakes, unknowingly,” said Misa Graff, an associate professor in epidemiology at the University of North Carolina and a genetics researcher.
In fact, that's already happening. In 2016, for example, research found that some Black patients had been misdiagnosed with a potentially fatal heart condition because they'd tested positive for a genetic variant thought to be harmful. That variant is much more common among Black Americans than white Americans, the research found, and is considered likely harmless among Black people. Misclassifications can be avoided if “even modest numbers of people from diverse populations are included in sequence databases,” the authors wrote.
The genetics research project in Charleston requires participants to complete an online consent form and submit a saliva sample, either in person at a designated lab or collection event or by mail. They are not paid to participate, but they do receive a report outlining their DNA results. Those who test positive for a genetic marker linked to cancer or high cholesterol are offered a virtual appointment with a genetics counselor free of charge.
Some research projects require more time from their volunteers, which can skew the pool of participants, Graff said, because not everyone has the luxury of free time. “We need to be even more creative in how we obtain people to help contribute to studies,” she said.
Moultrie said he recently asked project leaders to reach out to African American media outlets throughout the Palmetto State to explain how the genetics research project works and to encourage Black people to participate. He also suggested that when researchers talk to Black community leaders, such as church pastors, they ought to persuade those leaders to enroll in the study instead of simply passing the message along to their congregations.
“We have new ideas. We have ways we can do this,” Moultrie said. “We'll get there.”
Other ongoing efforts are already improving diversity in genetics research. At the National Institutes of Health, a program called “All of Us” aims to analyze the DNA of more than 1 million people across the country to build a diverse health database. So far, that program has enrolled more than 790,000 participants. Of these, more than 560,000 have provided DNA samples and about 45% identify as being part of a racial or ethnic minority group.
“Diversity is so important,” said Karriem Watson, chief engagement officer for the All of Us research program. “When you think about groups that carry the greatest burden of disease, we know that those groups are often from minoritized populations.”
Diverse participation in All of Us hasn't come about by accident. NIH researchers strategically partnered with community health centers, faith-based groups, and Black fraternities and sororities to recruit people who have been historically underrepresented in biomedical research.
In South Carolina, for example, the NIH works with Cooperative Health, a network of federally qualified health centers near the state capital that serve many patients who are uninsured and Black, to recruit patients for All of Us. Eric Schlueter, chief medical officer of Cooperative Health, said the partnership works because their patients trust them.
“We have a strong history of being integrated into the community. Many of our employees grew up and still live in the same communities that we serve,” Schlueter said. “That is what is part of our secret sauce.”
So far, Cooperative Health has enrolled almost 3,000 people in the research program, about 70% of whom are Black.
“Our patients are just like other patients,” Schlueter said. “They want to be able to provide an opportunity for their children and their children's children to have better health, and they realize this is an opportunity to do that.”
Theoretically, researchers at the NIH and the Medical University of South Carolina may be trying to recruit some of the same people for their separate genetics studies, although nothing would prevent a patient from participating in both efforts.
The researchers in Charleston acknowledge they still have work to do. To date, In Our DNA SC has recruited about half of the 100,000 people it hopes for, and of those, about three-quarters have submitted DNA samples.
Caitlin Allen, a program investigator and a public health researcher at the medical university, acknowledged that some of the program's tactics haven't succeeded in recruiting many Black participants.
For example, some patients scheduled to see providers at the Medical University of South Carolina receive an electronic message through their patient portal before an appointment, which includes information about participating in the research project. But studies show that racial and ethnic minorities are less likely to engage with their electronic health records than white patients, Allen said.
“We see low uptake” with that strategy, she said, because many of the people researchers are trying to engage likely aren't receiving the message.
The study involves four research coordinators trained to take DNA samples, but there's a limit to how many people they can talk to face-to-face. “We're not necessarily able to go into every single room,” Allen said.
That said, in-person community events seem to work well for enrolling diverse participants. In March, In Our DNA SC research coordinators collected more than 30 DNA samples at a bicentennial event in Orangeburg, South Carolina, where more than 60% of residents identify as Black. Between the first and second year of the research project, Allen said, In Our DNA SC doubled the number of these community events that research coordinators attended.
“I would love to see it ramp up even more,” she said.
——————————
By: Lauren Sausser
Title: Genetics Studies Have a Diversity Problem That Researchers Struggle To Fix
Sourced From: kffhealthnews.org/news/article/genetics-research-diversity-conundrum-black-participation-south-carolina/
Published Date: Thu, 25 Apr 2024 09:00:00 +0000
Did you miss our previous article…
https://www.biloxinewsevents.com/tire-toxicity-faces-fresh-scrutiny-after-salmon-die-offs/
Kaiser Health News
Tire Toxicity Faces Fresh Scrutiny After Salmon Die-Offs
Jim Robbins
Wed, 24 Apr 2024 09:00:00 +0000
For decades, concerns about automobile pollution have focused on what comes out of the tailpipe. Now, researchers and regulators say, we need to pay more attention to toxic emissions from tires as vehicles roll down the road.
At the top of the list of worries is a chemical called 6PPD, which is added to rubber tires to help them last longer. When tires wear on pavement, 6PPD is released. It reacts with ozone to become a different chemical, 6PPD-q, which can be extremely toxic — so much so that it has been linked to repeated fish kills in Washington state.
The trouble with tires doesn't stop there. Tires are made primarily of natural rubber and synthetic rubber, but they contain hundreds of other ingredients, often including steel and heavy metals such as copper, lead, cadmium, and zinc.
As car tires wear, the rubber disappears in particles, both bits that can be seen with the naked eye and microparticles. Testing by a British company, Emissions Analytics, found that a car's tires emit 1 trillion ultrafine particles per kilometer driven — from 5 to 9 pounds of rubber per internal combustion car per year.
And what's in those particles is a mystery, because tire ingredients are proprietary.
“You've got a chemical cocktail in these tires that no one really understands and is kept highly confidential by the tire manufacturers,” said Nick Molden, CEO of Emissions Analytics. “We struggle to think of another consumer product that is so prevalent in the world and used by virtually everyone, where there is so little known of what is in them.”
Regulators have only begun to address the toxic tire problem, though there has been some action on 6PPD.
The chemical was identified by a team of researchers, led by scientists at Washington State University and the University of Washington, who were trying to determine why coho salmon returning to Seattle-area creeks to spawn were dying in large numbers.
Working for the Washington Stormwater Center, the scientists tested some 2,000 substances to determine which one was causing the die-offs, and in 2020 they announced they'd found the culprit: 6PPD.
The Yurok Tribe in Northern California, along with two other West Coast Native American tribes, have petitioned the Environmental Protection Agency to prohibit the chemical. The EPA said it is considering new rules governing the chemical. “We could not sit idle while 6PPD kills the fish that sustain us,” said Joseph L. James, chairman of the Yurok Tribe, in a statement. “This lethal toxin has no place in any salmon-bearing watershed.”
California has begun taking steps to regulate the chemical, last year classifying tires containing it as a “priority product,” which requires manufacturers to search for and test substitutes.
“6PPD plays a crucial role in the safety of tires on California's roads and, currently, there are no widely available safer alternatives,” said Karl Palmer, a deputy director at the state's Department of Toxic Substances Control. “For this reason, our framework is ideally suited for identifying alternatives to 6PPD that ensure the continued safety of tires on California's roads while protecting California's fish populations and the communities that rely on them.”
The U.S. Tire Manufacturers Association says it has mobilized a consortium of 16 tire manufacturers to carry out an analysis of alternatives. Anne Forristall Luke, USTMA president and CEO, said it “will yield the most effective and exhaustive review possible of whether a safer alternative to 6PPD in tires currently exists.”
Molden, however, said there is a catch. “If they don't investigate, they aren't allowed to sell in the state of California,” he said. “If they investigate and don't find an alternative, they can go on selling. They don't have to find a substitute. And today there is no alternative to 6PPD.”
California is also studying a request by the California Stormwater Quality Association to classify tires containing zinc, a heavy metal, as a priority product, requiring manufacturers to search for an alternative. Zinc is used in the vulcanization process to increase the strength of the rubber.
When it comes to tire particles, though, there hasn't been any action, even as the problem worsens with the proliferation of electric cars. Because of their quicker acceleration and greater torque, electric vehicles wear out tires faster and emit an estimated 20% more tire particles than the average gas-powered car.
A recent study in Southern California found tire and brake emissions in Anaheim accounted for 30% of PM2.5, a small-particulate air pollutant, while exhaust emissions accounted for 19%. Tests by Emissions Analytics have found that tires produce up to 2,000 times as much particle pollution by mass as tailpipes.
These particles end up in water and air and are often ingested. Ultrafine particles, even smaller than PM2.5, are also emitted by tires and can be inhaled and travel directly to the brain. New research suggests tire microparticles should be classified as a pollutant of “high concern.”
In a report issued last year, researchers at Imperial College London said the particles could affect the heart, lungs, and reproductive organs and cause cancer.
People who live or work along roadways, often low-income, are exposed to more of the toxic substances.
Tires are also a major source of microplastics. More than three-quarters of microplastics entering the ocean come from the synthetic rubber in tires, according to a report from the Pew Charitable Trusts and the British company Systemiq.
And there are still a great many unknowns in tire emissions, which can be especially complex to analyze because heat and pressure can transform tire ingredients into other compounds.
One outstanding research question is whether 6PPD-q affects people, and what health problems, if any, it could cause. A recent study published in Environmental Science & Technology Letters found high levels of the chemical in urine samples from a region of South China, with levels highest in pregnant women.
The discovery of 6PPD-q, Molden said, has sparked fresh interest in the health and environmental impacts of tires, and he expects an abundance of new research in the coming years. “The jigsaw pieces are coming together,” he said. “But it's a thousand-piece jigsaw, not a 200-piece jigsaw.”
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
——————————
By: Jim Robbins
Title: Tire Toxicity Faces Fresh Scrutiny After Salmon Die-Offs
Sourced From: kffhealthnews.org/news/article/tire-toxicity-salmon-die-offs-research-6ppd/
Published Date: Wed, 24 Apr 2024 09:00:00 +0000
Did you miss our previous article…
https://www.biloxinewsevents.com/ftc-chief-says-tech-advancements-risk-health-care-price-fixing/
-
Mississippi News7 days ago
What this means for local schools
-
228Sports4 days ago
From Heartbreak to Hoop Dreams: Pascagoula Panthers Springboard from Semifinal Setback to College Courts
-
Mississippi News4 days ago
2 dead, 6 hurt in shooting at Memphis, Tennessee block party: police
-
Mississippi News7 days ago
Willis Miller sentenced to 45 years in prison, mandatory
-
Mississippi News4 days ago
Forest landowners can apply for federal emergency loans
-
Mississippi Today7 days ago
The unlikely Mississippi politician who could tank Medicaid expansion
-
Mississippi News6 days ago
Burnsville man arrested in Prentiss County on drug related charges
-
Mississippi News3 days ago
Cicadas expected to takeover north Mississippi counties soon